


Diabetes has wide-ranging effects on your body. It can be a dangerous health issue, but the good news is that you aren’t powerless when it comes to this disease!
There are actions within the realm of your control that can help you manage the disease and reduce your risk of serious medical complications. Let’s take a look at some of the diabetic lifestyle changes you can make to keep the disease in check:
Better eating. As you likely know, diabetes is the result of elevated blood sugar levels. One of the keys to managing the disease is to focus your diet on healthy eating. Before we delve into what actually constitutes “healthy eating,” here’s a quick tip that can help you find success – Instead of labeling food as “good” and “bad,” think and speak about your dietary habits in the context of “I am choosing to/not to eat _____.” This is an empowering frame of reference. Also, when you affix the “good” and “bad” labels, it can lead to a downward spiral if you go off the track.
More specifically, though, you need to base your diet on veggies, lean meats, low-fat dairy products, legumes, and nuts. (Actually, if you think about it, this is just a smart dietary plan for anyone, diabetic or not!) Contrary to what we have been told, it is best to avoid whole grains and fruit as they excessively raise blood sugar levels. Avoid sugary beverages and, instead, drink lots of water and unsweetened tea. Coffee can be fine, but don’t use sugar-laden syrups. If you get coffee from places like Starbucks, ask for sugar-free options.
Exercise. It is difficult to overstate just how important exercising is for you. The physical, mental, and emotional benefits are countless, including diabetes management. The cardiovascular benefits of regular exercise are particularly important as you manage your diabetes.
Before you begin any kind of workout program, make sure you consult with your primary care physician and our office (especially if it’s been a long time since you last worked out). We can determine if there are any existing or potential issues you need to be aware of. Also, we can provide recommendations for exercises that will be best for you.
Foot care. Given all the issues diabetes can cause for your body, it can be easy to forget how the disease affects the health of your feet. This is not something you want to overlook, though!
Diabetes contributes to both nerve damage (neuropathy) and weakened blood flow (peripheral arterial disease). In turn, these can lead to dangerous situations for your feet, like diabetic ulcers and Charcot foot.
Damaged nerves can leave you unable to feel when damage—including cuts, scrapes, ingrown toenails, and calluses—has been sustained to your lower limbs. Those might be relatively minor problems for someone with normally functioning nerves and immune systems, but they can break down, become infected, and lead to gangrene. Unfortunately, the only way to treat gangrene is amputation. A proper diabetic foot care plan is centered on prevention and protection for your lower limbs, along with daily inspection to catch issues early. If you would like assistance putting yours together, we will be glad to help.
Regular appointments. If you don’t already, make sure you come in to see us roughly every two months. Regular checkups are important so we can catch issues at their earliest, most-treatable stages. We can also review your daily inspection checklist and make sure everything is going well. Of course, this also gives you the chance to ask questions to a medical professional.
For additional information on diabetic foot care, the services we offer, or to request an appointment with our Bloomington, IN podiatrist office, give us a call at (812) 333-4422.
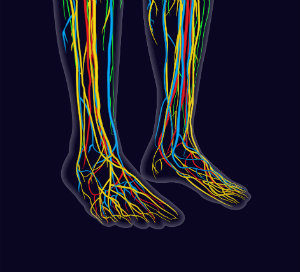 We treat patients for many different conditions, but one of the most concerning is nerve damage in feet. Neuropathy is a condition wherein your peripheral nerves—the ones responsible for recording information and communicating it back to the spinal column and brain (your central nervous system)—are damaged. This can become an emergency situation when an untreated minor cut or sore breaks down over time and becomes an ulcer.
We treat patients for many different conditions, but one of the most concerning is nerve damage in feet. Neuropathy is a condition wherein your peripheral nerves—the ones responsible for recording information and communicating it back to the spinal column and brain (your central nervous system)—are damaged. This can become an emergency situation when an untreated minor cut or sore breaks down over time and becomes an ulcer.
Neuropathy is a concern no matter where in the body it develops, but nerve damage in the feet can be particularly alarming for a couple of reasons. First, your feet endure tremendous force loads on a daily basis, which puts them at heightened risk for injury and medical conditions. Second, feet are generally not particularly visible. Our lower limbs are often covered in socks and shoes, plus they are the furthest points on the body from our eyes. This means you have to be vigilant to catch those issues that can become medical emergencies if you have neuropathy!
Whereas neuropathy is commonly associated with diabetes—and rightfully so given that 60-70 percent of diabetic individuals will develop nerve damage during their lifetime—there are several other potential sources, including:
If you have sustained nerve damage in your feet that is causing problems like burning, tingling, or painful sensations, or you are unable to feel anything, come see us here at our Bloomington, IN office. We will determine the root cause of the problem and then create an effective treatment plan for you. If diabetes is responsible, we can help you develop a diabetic foot care plan to prevent issues from arising in the first place.
Call us at (812) 333-4422 for more information, or assistance in scheduling an appointment that works for you. You can also take advantage of our online form to contact us right now.
We may have just gotten out of National Diabetes Awareness month, but this disease needs to be given attention all year long. The number of Americans living with diabetes is staggering (29 million) and, even more concerning, it’s climbing. Effects on the body from the disease can be found, literally, from head to toe. It might be easy to think about ones like increased risk of heart attack, kidney failure, and potential blindness, but it would be a mistake to look past the link between diabetes and foot health.
Diabetes is a condition that develops on account of excessive blood sugar levels in the bloodstream. This happens when the body either doesn’t produce enough insulin—a hormone that allows the body to properly absorb and use sugar (glucose)—or it is unable to use the insulin effectively. In some cases, both of these problems exist at the same time.
The excess glucose in the blood can cause problems for most of the body’s organs and nerves. As we look at how diabetes affects foot health, skin is a central organ in the big picture.
Changes to the skin in the lower body can be an indication of a diabetic condition. These include more frequent callusing, increased itching sensations, loss of body hair, and shiny, thinning skin. Callusing is of particular concern since a callus can break down over time and become a diabetic ulcer.
Diabetic ulcers are extremely concerning. Ulceration is a breakdown of body tissue, which often results in open sores and wounds. These enable microorganisms (bacteria, fungus) to enter the body. Diabetes impairs the body’s ability to fight off infection, and a potentially serious situation can arise – gangrene. Gangrene is tissue death that cannot be treated. Instead, dead tissue needs to be removed in order to prevent it from spreading. Accordingly, this is a leading cause of lower limb amputations.
Two major conditions that play a role in diabetes and foot health are diabetic neuropathy and peripheral arterial disease (PAD). Neuropathy refers to the nerve damage that has taken place on account of the heightened glucose levels. This can leave an affected individual unable to tell when an issue exists, which then can lead to the problem worsening. PAD is a condition wherein blood vessels have become constricted and do not allow tissues to receive the oxygenated blood they need.
Diabetes can lead to severe consequences and problems for your lower limbs. If you live with this disease, come and see us as soon as possible so we can help you create a diabetic foot care plan to keep you safe. Schedule your appointment with our Bloomington, IN office by calling (812) 333-4422.